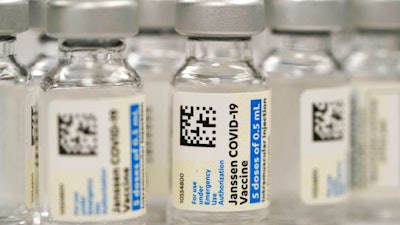
U.S. regulators are allowing the release of about 10 million doses of Johnson & Johnson's COVID-19 vaccine from a troubled Baltimore factory, but many more doses can't be used and must be thrown out.
The Food and Drug Administration announced Friday that it had determined that two batches could be released from the plant, which is owned by Emergent BioSolutions and has been shuttered for eight weeks. But it said several other batches are not suitable for use and additional batches are still under review.
The agency wouldn't specify the size of those batches or why they can't be used, but a person familiar with the decision told The Associated Press that they could have yielded tens of millions of doses and that they possibly were contaminated. Another person familiar with the situation said the doses to be discarded were made about the same time as a vaccine batch equal to about 15 million doses that was contaminated earlier this year and thrown out.
Neither person was authorized to release details about the decision and spoke to the AP on condition of anonymity.
J&J and Emergent wouldn't give any details on the size of the batches that are usable, nor those being discarded.
The two batches from the factory known as Bayview can be used in the U.S. or exported to other countries. They are the first J&J vaccines from Bayview approved for use.
The FDA said if any of the vaccine is exported, J&J and Emergent must allow the agency to share information about the manufacture of those batches confidentially with regulators in other countries.
The FDA statement implied that the batches didn't meet all of the agency's manufacturing quality standards. “This review has been taking place while Emergent BioSolutions prepares to resume manufacturing operations with corrective actions to ensure compliance with the FDA’s” manufacturing requirements, Dr. Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, said in a statement.
The agency said the vaccines are “critically needed,” given the current public health emergency, and that it made the decisions after reviewing records and the results of quality testing.
The FDA, however, stopped short of allowing the plant to restart vaccine production. The agency said it was working through issues there with J&J and Emergent BioSolutions management.
Emergent is one of several J&J contractors that produce its one-shot vaccine in bulk. The concentrated vaccine then is shipped to other factories for final steps, including diluting them to the correct strength, putting them in vials and packaging them up.
Roughly 100 million doses made from bulk vaccine produced at Emergent’s factory, including those just approved for use, had been set aside for additional review by FDA staff after factory employees accidentally contaminated an earlier batch.
That contamination led the FDA to shut down the factory in mid-April and send in a team of inspectors. They spent a week going through the factory and reviewing security camera footage that showed employees carelessly handling vaccine materials. The inspectors reported unsanitary conditions, poorly trained employees and other problems.
The lapses have hampered J&J's efforts to be a major player in vaccinating people, particularly in remote areas and poor countries, given that it’s the only drugmaker with an authorized vaccine that only requires one dose and standard refrigeration. It's also cheaper than some other vaccines.
The productions problems have forced J&J to import millions of doses from its factory in the Netherlands to the U.S. and to miss supply commitments.
Emergent’s factory had a history of FDA citations for problems including mold, dirty walls and floors, poorly trained employees and an inadequate strategy to prevent contamination, yet it was given a huge role in COVID-19 vaccine production by the Trump administration. Emergent was handed a lucrative contract to make many millions of COVID-19 vaccines for both J&J and AstraZeneca at the Bayview factory.
Emergent’s chief executive has blamed the contamination and other problems on the complexity of scaling up the factory in just months to make two different vaccines.
The Biden administration is working to find a different American manufacturing partner for the British drugmaker, which has yet to request authorization to distribute it in the U.S.
___






















